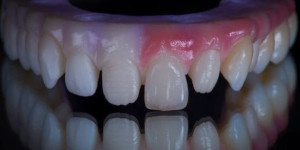
Zirconia offers an excellent balance of strength and esthetics for crowns and bridges, especially in posterior regions that bear high bite forces. It is chemically inert, lustrous, and available in translucent grades that can be used monolithicallyor veneered with porcelain for enhanced anterior esthetics. Typical flexural strength for 3Y-TZP zirconia is ~900–1200 MPa (lab/manufacturer dependent). With proper design and finishing, zirconia restorations show low rates of crack propagation and chipping.
Key points for Zirconia case selection and prep
Tooth preparation: Reduced thickness is possible versus many ceramics, but respect manufacturer minimums (occlusal ~0.8–1.0 mm; axial ~0.6–0.8 mm depending on grade).
Customization: Zirconia is CAD/CAM-millable and can be shaded, stained, and glazed to match natural teeth (it is not malleable like metal).
Biocompatibility & comfort: Low thermal conductivity helps limit temperature-related sensitivity; tissue response is generally favorable.
Implant utility: High strength makes it suitable where interocclusal space is limited, including full-arch frameworks or posterior implant crowns.
Clinical considerations for Zirconia
Monolithic zirconia reduces veneer-chipping risk; veneered zirconia can achieve superior translucency in the esthetic zone but is more chip-prone under high shear.
Longevity commonly exceeds 5+ years with high survival when occlusion is balanced and surfaces are well polished.
Follow manufacturer guidance on material grade, thickness, and finishing to optimize toughness and wear behavior.
Bottom line: as translucency increases, flexural strength and fracture toughness decrease—choose the zirconia grade (3Y/4Y/5Y) to balance esthetics with load demands for each case.